Link between viruses and abnormalities in pregnancy
The link between adverse pregnancy outcomes and infectious disease is well known (1,2,3). Infections in pregnancy can cause miscarriage, preterm birth and fetal death in utero (1,2,3).
A specific link between some viral infections in pregnancy and birth defects in newborns has also been established. In 1941, Australian Norman Gregg determined that maternal rubella caused birth defects by linking the infection to congenital deafness (4).
The recent observation of an increased risk of microcephaly in newborns whose mothers acquired Zika virus in pregnancy has again brought the issue of viral infections and pregnancy to world attention (5,6).
What is microcephaly?
Microcephaly literally means small head, and occurs when the head circumference of a newborn is below the 3rd centile, meaning 97% of all other newborn babies have a head that is larger in size and only 3% have a head size the same or smaller. Head circumference is affected by age, gender, ethnicity and culture, so it is important to take accurate measurements and apply these to validated local charts to determine the correct centiles and confirm the diagnosis (7)
The significance of a small head is obvious. It suggests the development of the brain has been delayed or impaired. A smaller head means the baby might have fewer neurones (brain cells), synapses and myelin coated axons (connectors between brain cells) capable of transmitting and processing information around the nervous system. This delay or lack of integration within the brain is associated with an increased risk of developmental delay and intellectual disability.
However, in some cases a small head may be normal. After all, some people have small heads and other people large ones. That is why there are differences in hat size.
What is Zika virus?
Zika virus is carried by Aedes mosquitoes. The virus was first identified in Uganda in 1947. The first cases involving transmission to humans were reported from Africa and Asia, however it was not until 2007 that an outbreak in Micronesia brought the virus to the attention of authorities (5).
The clinical presentation is usually mild with a fever, rash and watery eyes. Some people report fatigue, malaise and muscle pains. Symptoms usually last less than a week. The incubation period, or time between being bitten by an affected mosquito and the onset of symptoms, is not yet clear (6).
However, it is the link to abnormalities in pregnancy that has caused international concern.
Zika virus and pregnancy
There have been a number of outbreaks of Zika virus around the world in recent years, the most recent before the current outbreak was in Micronesia in 2013.
However, the 2015 Brazilian outbreak and epidemiological association with microcephaly has been the precipitating factor to hone world attention onto the virus.
What to do if you’re pregnant and worried about Zika?
Firstly, if you live in a region where the Zika virus has not been detected, you can be reassured. There is no good evidence of person to person transmission, although the first case of potential sexual transmission of the virus has been noted.
However, if you live in an affected area, or have travelled to such an area, then read on.
The general principles of management are as follows
- Prevention
- Diagnosis
- Management
- Follow up
Prevention
As there is no vaccine or cure for the infection, the current focus of management is prevention.
The key to prevention is to avoid being bitten by an Aedes mosquito in a region where the virus circulates. Unfortunately this includes many regions in Africa, the Americas, Asia and the Pacific (6). Pregnant travellers should avoid these regions.
If you live in an endemic region, the principle of management is a public health approach.
Public health strategies involve reducing the capacity of mosquitoes to breed by controlling breeding grounds, and by adapting local lifestyles to minimise the risk of being bitten. This can include changing the way you dress, using topical repellants, sleeping under nets and erecting physical barriers such as screens on windows and doors.
Diagnosis
If a pregnant woman suspects she may have contracted Zika virus infection she should immediately seek medical attention.
General practitioners should refer the woman to an obstetrician or clinical microbiologist.
Diagnosis of infection is made by blood sample tested using PCR for viral isolation. A positive result should be double checked as there is the potential for cross reactivity with other viral infections such as dengue, yellow fever and West Nile fever (6).
Management
The primary infection may be easily managed using supportive therapy such as paracetamol to reduce the risk of fever and manage muscle pains. It is important to keep well hydrated and women should be encouraged to drink water to keep their urine from being concentrated. Rest and adequate diet are also important to improve the body’s capacity to fight infection.
If a blood test confirms infection, then referral to a maternal fetal medicine specialist is recommended.
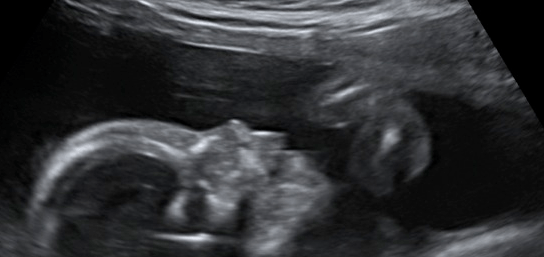
A tertiary level ultrasound can determine if there is any discordance between the centiles of growth of the fetal head compared to other parts of the baby such as its abdominal circumference or femur bone length in the leg. An amniocentesis may also be performed and a sample of amniotic fluid removed for PCR analysis. A positive result will confirm intrauterine infection.
Serial ultrasound examination can help document the progress of fetal growth and look for any other abnormalities.
Once all the information is available, women should be carefully counselled according to the specific findings in their case. If tests are negative, they can be reassured. If positive, counselling will depend upon the specific positive findings.
Follow up
Any newborn born to a women with Zika viral infection in pregnancy should be enrolled into a follow up program. This is important as we currently lack sufficient information to provide counselling about the long term consequences of infection.
It may be that most children born are normal and follow a normal developmental pathway. We do not know the answer to this question.
However, if a child does have a problem, then a follow up program will ensure the problem is detected early, and interventions can be applied to improve outcomes. By example, if a learning problem was diagnosed, specialist education interventions could be started. In some countries, such as Australia, parents may be eligible for funds to support early intervention disability services.
Establishing a database of long term outcomes is critical to improve the counselling for affected parents. As more cases are added to the data base, clinicians will be able to provide parents with more accurate advice about outcomes.
Summary
The association between Zika virus and microcephaly is a new development. There is still insufficient information to establish this is causal, and other explanations still need to be excluded.
However, the epidemiological link has resulted in a global effort focussed on prevention and management of Zika virus infection in pregnancy.
References
- Mendz GL, Kaakoush NO, Quinlivan JA Bacterial aetiological agents of intra-amniotic infections and preterm birth in pregnant women. Frontiers in Cellular Infection and Microbiology. 2013, 3: 58. doi: 10.3389/fcimb.2013.00058
- Quinlivan JA, Kaakoush NO, Mendz GL. Acinetobacter Species Associated with Spontaneous Preterm Birth and Histological Chorioamnionitis. British Journal of Medicine & Medical Research, 2014; 4(33): 5293-5297.
- Mendz GL, Petersen R, Quinlivan JA, Kaakoush NO. Potential involvement of Campylobacter curvus and Haemophilus parainfluenzae in preterm birth. BMJ Case Reports 2014: published online 1 October 2014, doi:10.1136/bcr-2014-205282.
- Lancaster PA. Causes of birth defects: lessons from history. Congen Anom. 2011 ;51(1) :2-5.
- Ioos S, Mallet H, Leparc-Goffart I et al. Macdecine et Maladies Infectieuses. 2014; 44(7). DOI: 10.1016/j.medmal.2014.04.008.
- World Health Organisation. Zika virus. Published by WHO in January 2016. Accessed on 6 February 2016. Available from http://www.who.int/mediacentre/factsheets/zika/en/
- Woods CG, Parker A. Investigating microcephaly. Arch Dis Child 2013; 98:707.
Daytime active mosquito carrier of Zika Virus
Thanks for this very interesting summary of Zika virus in pregnancy. Of note, the Aedes aegypti mosquito is active during the daytime as well as evenings therefore it is imperative that pregnant women cover up their arms and legs and wear insect repellant to reduce the risk of being bitten. It also likes shady and cool areas example under your house.
If the mother proves positive to Zika on serology but the anatomy ultrasound scan is normal, is it worthwhile doing an Amniocentesis?
LikeLiked by 1 person
It may be possible to detect Zika virus on PCR and this may help with counselling. A negative Zika PCR reassures against current intrauterine infection. However, it carries the risk of pregnancy loss associated with amniocentesis. A negative amniocentesis doesn’t mean infection may not happen in the future, especially if the mother has an ongoing high viral load in her blood stream. A positive amniocentesis also doesn’t necessarily mean an affected baby, especially with a normal tertiary ultrasound examination. Ultimately it requires detailed counselling of all the advantages and disadvantages.
LikeLike